

The Toxic Drug Poisoning Crisis through the
DPIE Framework in British Columbia
Abstract:
The toxic drug poisoning crisis, commonly referred to as the opioid crisis, remains a severe public health challenge in British Columbia, with persistent overdose fatalities across the province. This study introduces a macro-level framework, DPIE, that decomposes overdose deaths into the population at risk, the incidence of overdose, and the effectiveness of intervention. Using municipality-level data, we analyze opioid-related mortality across British Columbia from 2016 to 2024. Results show that increases in overdose incidence have been the primary driver of rising mortality since 2019, while changes in the population at risk have played a comparatively minor role. At the regional level, Northern Health recorded the highest death rate in 2024 (124.5 per 100,000 population at risk), whereas Fraser Health exhibited the lowest rate (47.8 per 100,000), followed closely by Vancouver Coastal Health. City-level analysis reveals even greater heterogeneity: Victoria and Langley (City) experienced high mortality and fatality rates driven largely by elevated incidence, while Surrey recorded many overdose cases but very low mortality, indicating relatively high intervention effectiveness. Overall, the findings suggest that overdose mortality is shaped not only by the presence of support services, but by their accessibility and by broader systemic conditions that influence overdose risk. The DPIE framework provides an evidence-based tool for disentangling these mechanisms and for evaluating and targeting overdose policy interventions. Coordinated action across municipal, provincial, and federal levels remains essential to address the ongoing crisis effectively.
Keywords: toxic drug poisoning crisis, opioid crisis, overdose deaths, population at risk, incidence rate, intervention efficacy, prevention and consumption sites, complex care housing
The toxic drug poisoning crisis has emerged as one of Canada’s most pressing public health emergencies, with British Columbia (BC) experiencing the highest number of opioid-related deaths nationwide (Government of Canada, 2024). Since the BC Provincial Health Officer declared a public health emergency in April 2016 (Panagiotoglou, 2022), the province has recorded nearly 50,000 opioid-related deaths, alongside thousands of hospitalizations and emergency responses (Government of Canada, 2024).
The crisis exerts a toll on healthcare systems, social services, and the community at large. Across BC’s five health authorities, Fraser Health, Interior Health, Island Health, Northern Health, and Vancouver Coastal Health, 176 municipalities are impacted, with deaths concentrated among adults aged 19–59, accounting for approximately 88% of toxic drug poisoning deaths (BC Coroners Service, 2025).
Despite the implementation of various harm reduction initiatives and support services, the incidence of overdose fatalities continues to rise. Factors such as the increasing prevalence of fentanyl (Tobias et al., 2024), socioeconomic vulnerabilities (Carrière et al., 2021), and limited mental health support (Akunna et al., 2024) have exacerbated the crisis. Although British Columbia introduced one of North America’s most comprehensive overdose response strategies prior to the COVID-19 pandemic (McNeil et al., 2022), the pandemic disrupted services for vulnerable populations (Tobias et al., 2024). Addressing the opioid crisis requires more than reactive emergency responses; it demands a coordinated, proactive, and comprehensive approach involving multiple sectors, including all levels of government, healthcare, education, and social services. Public interventions must target the broader social determinants of health, including poverty, homelessness, and mental health, while also strengthening support systems to reduce overdose mortality.
To contribute to this broader understanding, this research introduces and applies a new analytical framework in which opioid-related deaths (D) are modeled as the product of three multiplicative factors, namely, the population at risk (P), the incidence rate of opioid use (I), and the effectiveness of intervention (E). Formally, Deaths = P × I × E. While “E” refers to the probability of death per overdose case, commonly known as the case fatality rate (CFR), it serves as a proxy for the overall effectiveness of intervention. In this framework, lower values of E indicate more effective intervention. In this framework, lower values of E indicate more effective intervention, reflecting higher survival conditional on an overdose occurring. In the remainder of this paper, the term “effectiveness of intervention” is used instead of the epidemiology term CFR. The framework mirrors the logic of the IPAT identity, where environmental impact depends on factors such as the size of the population, the affluence of society, and the technology available to address environmental crises (Ehrlich & Holdren, 1971). Just as the IPAT framework helps pinpoint the drivers of environmental degradation, the DPIE identity can guide policy analysis by identifying the key drivers of opioid fatality. For example, if the at-risk population (P) and the incidence rate (I) increase, the death rate can only decline if the effectiveness of intervention improves, meaning that (E) is reduced fast enough to offset the growing population at risk and the incidence rate. As in Waggoner and Ausubel (2002), “P” and “I” represent the sustainability challenges society faces, while E is the sustainability lever. Although with proper policy in place, “I” can become a lever instead of a challenge, as will be discussed. Reinforcing this approach, Wakeland et al. (2022) developed a dynamic simulation of the U.S. opioid crisis, demonstrating how delays in implementing effective interventions can exacerbate mortality over time. Together, these frameworks support a structured, evidence-based approach to understanding and mitigating one of North America’s most devastating public health crises.
By applying the model to secondary data from multiple municipalities, this study aims to:
The following sections describe the D = PIE framework in detail and present empirical results across BC’s health authorities, followed by a discussion of systemic barriers, successful strategies, and long-term solutions.
The DPIE framework provides an attribution-based interpretation of observed opioid-related deaths, describing how the number of deaths in a given period can be decomposed into contributions from the population at risk, the incidence rate of overdose, and the effectiveness of intervention. As an identity-based decomposition, DPIE does not establish causal relationships; rather, it identifies which components account for most of the change in observed mortality across time and communities. Using this framework, researchers can identify which components dominate changes in deaths over time, and it can also serve as a scenario-based assessment tool to help predict the expected number of deaths in the future. Municipalities can use the framework to develop and shape policy and create awareness about how resources may be used more effectively by interpreting patterns in exposure and intervention effectiveness over time.
The framework is named DPIE and is an identity expressed mathematically as follows:
\(D_{i,t} \equiv P_{i,t}I_{i,t}E_{i}\)
(1)
where, \(D_{i,t}\) represents deaths in community i at a given year t the observed outcome),\(D_{i,t}\) is the population at risk in community i at time t (i.e., the potential exposure to death), \(I_{i,t} = \frac{C_{i,t}}{P_{i,t}}\) represents the number of new opioid overdose cases \(C_{i,t}\) per unit of population at risk (i.e., the incidence rate representing exposure or burden of overdose towards death), and \(E_{i} = \frac{D_{i,t}}{C_{i,t}}\) represents the effectiveness of intervention based on the fatalities to number of new overdose cases. The incidence rate, \(I_{i,t}\), in epidemiology, represents the risk of developing a particular disease over a given period. It is calculated as the number of new cases during the specified time divided by the population at risk. In the context of opioid overdoses, the incidence rate is the risk of experiencing an overdose within a period, defined as \(I_{i,t}\), where \(C_{i,t}\) is the number of new overdose cases in community i at time t, and \(P_{i,t}\) is the population at risk. Overdose cases (C) specifically refer to overdose events occurring within the community. These cases are collected from emergency response data, including records from the British Columbia Emergency Health Services (BCEHS).
The effectiveness of intervention \(E_{i,t}\) measures the probability of death among those diagnosed with a specific disease, represented as \(\frac{D_{i,t}}{C_{i,t}}\). A key challenge is the rising population at risk due to overall population growth in many communities. To reduce overdose deaths, policymakers and communities must focus on lowering the incidence \(I_{i,t}\) and improving intervention effectiveness (reducing \(E_{i}\)) at a faster rate than the increase in the at-risk population.
This macro model does not provide a causal explanation of why each variable is increasing or decreasing. The identity will always be true, but it functions as an accounting framework to track patterns over time. Although it may appear that each factor is independent, in practice the variables are inter-connected. The population at risk is largely exogenous at the community level, but we can analyze the incidence rates by looking at what kind of initiatives, funding, education, programs, and resources are being implemented to reduce the incidence rate and increase the effectiveness rate to offset the increased population at risk. Reducing the levers of exposure and increasing effectiveness can lower total deaths, while the opposite conditions may exacerbate the crisis.
Furthermore, the approach can be used to conduct scenario-based assessments, such as setting community targets to reduce deaths by 2030 to 10% of 2025 levels, based on population-at-risk trends and the policy changes required to reduce both incidence rates and fatality probabilities. Once this analysis is conducted, a cost-benefit assessment can evaluate the value of health benefits from lives saved relative to the cost of interventions.
The areas of interest include the five British Columbia health authorities operating across sixteen municipalities from 2016 to 2024. The sixteen cities were chosen based on available data within the different health authorities in British Columbia. Each health authority consistently captures the data; however, cities differ in their experiences and dynamics related to the overdose crisis, which impacts the number of deaths, interventions, exposure levels, and access to services. As a result, the municipal heterogeneity affects regulated and unregulated cases and deaths in different ways based on local responses, priorities, and interventions.
Confirmed unregulated drug toxicity deaths were obtained from the British Columbia Coroners Service interactive Power BI dashboard (“Unregulated Drug Deaths – Township of Injury”), which is periodically updated as investigations are completed. Death data were accessed and downloaded on December 24, 2025. Emergency overdose response volumes were drawn from British Columbia Emergency Health Services (BCEHS) public reporting tables (“MPDS Card 23 Events: Overdose Response in BC Communities; Top Communities, 2016–2024”), downloaded on December 24, 2025. These data represent yearly counts of overdose and poisoning calls attended by paramedics. Population at risk (ages 19–59) was derived from BC Stats sub-provincial population projections (2024 edition), accessed on December 24, 2025.
Counts of supervised consumption and overdose prevention sites were obtained from the BC Centre for Disease Control (BCCDC). Because several sources are updated retrospectively, all results reflect the data versions available on the stated access date.
All analyses use annual measures of deaths (D), overdose cases (C), and population at risk (P) aggregated by municipality and year, so that each observation corresponds to a municipality–year. The population at risk (P) consists of individuals aged 19–59. The incidence rate and effectiveness of intervention are calculated using aligned annual data on population size, overdose cases, and deaths derived from the administrative sources described above. These variables form a consistent dataset across municipalities and years for application of the DPIE framework.
Figure 1 shows observed trends in British Columbia's incidence rate (per 1,000 cases, shown in black) and the number of deaths (per 1,000 cases, shown in dark red) from 2016 to 2024 aggregated across the 16 cities. Over this period, there is an upward trend in the incidence rate, indicating an increased risk of exposure to the opioid crisis for those in the 19–59 age group. This increase implies that overdose cases are rising faster than the population at risk. In addition, the intervention efficacy rate also follows an upward path, but at a slower pace than the increase in overdose incidence. Therefore, both rising exposure to overdose and weaker intervention effectiveness contribute to increasing deaths.
During the pre-COVID-19 period, the incidence rate was relatively stable, while the intervention efficacy measure shows more volatility. However, continuing into the COVID-19 period, both the incidence and mortality rates increased and peaked between the 2022 and 2023 period, which suggests that the pandemic played a role in worsening the crisis during this period.
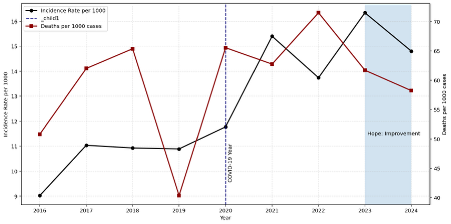
Figure 1: Trends in overdose incidence and mortality in 16 B.C. cities, 2016–2024 (Figure generated by the author using Spyder 6)
Table 1 presents opioid-related mortality and supervised consumption site availability across British Columbia’s five regional health authorities. Fraser Health, with the largest at-risk population (ages 19–59), recorded the lowest death rate at 48.4 per 100,000 population at risk and operated 11 supervised consumption sites, equivalent to 0.86 sites per 100,000 at-risk individuals. Vancouver Coastal Health, with 1.31 sites per 100,000 population at risk, had the second-lowest death rate at 73.5 per 100,000. Moving away from lower mainland, mortality rates increase substantially. Interior Health and Island Health exhibited higher death rates (90.2 and 97.1 per 100,000, respectively), despite having greater site density (1.98 and 1.70 sites per 100,000 population at risk, respectively). Northern Health, with just one site across 48 municipalities and the lowest site density (0.60 per 100,000 population at risk), reported the highest mortality rate at 126.9 per 100,000.
| Health Authority | Municipalities | Population at Risk 19-59 (2024 est.) | Prevention & Consumption Sites | Sites per 100,000 Population at Risk | Unregulated Drug-Related Deaths (2024) | Deaths per 100,000 Population at Risk |
|---|---|---|---|---|---|---|
| Fraser | 20 | 1,284,254 | 11 | 0.86 | 622 | 48.4 |
| Interior | 68 | 453,562 | 9 | 1.98 | 409 | 90.2 |
| Island | 28 | 471,916 | 8 | 1.70 | 458 | 97.1 |
| Northern | 48 | 166,258 | 1 | 0.60 | 211 | 126.9 |
| Vancouver Coastal | 12 | 836,944 | 11 | 1.31 | 615 | 73.5 |
Note: Population at risk is estimated as individuals aged 19–59 in each health authority, based on BC Stats (2024) projections. Death data reflect confirmed unregulated drug toxicity deaths reported by the BC Coroners Service Power BI Dashboard (accessed December 24, 2025). Site counts are from the BC Centre for Disease Control (BCCDC) as of 2024. Municipalities refer to incorporated local governments within each health authority.
Table 2 presents 2024 opioid-related mortality for the 16 cities in British Columbia, disaggregated by health authority to detect variation within regions. Each city is listed with its total population, population at risk (ages 19–59), number of overdose cases, and deaths. From these values, three metrics were calculated using the DPIE model: incidence (I), defined as the proportion of the at-risk population experiencing an overdose; effectiveness (E), interpreted as the probability of death given an overdose; and deaths per 100,000 population. The results reveal wide variation across cities. Langley (City) within Fraser Health Authority and Victoria within Island Health report the highest incidence rates of overdose among the population at risk (4.3% and 3.8%, respectively). Langley and Victoria also have the highest death rates in the province (217.7 and 262.5 per 100,000, respectively). The lowest incidence rate occurs in Richmond at 0.3%, which also reports one of the lowest death rates (17.9 per 100,000).
In terms of intervention effectiveness, Burnaby and Kamloops have the highest probability of death per overdose case (7.7% and 7.5%, respectively), while the most favourable intervention effectiveness is observed in Chilliwack (3.5%).
| City | Health Authority | Population | Population at Risk | Overdose | Deaths | Incidence | Intervention | Deaths |
|---|---|---|---|---|---|---|---|---|
| Abbotsford | Fraser | 175,087 | 96,453 | 1,501 | 75 | 0.016 | 0.050 | 77.8 |
| Burnaby | Fraser | 298,986 | 182,959 | 739 | 57 | 0.004 | 0.077 | 31.2 |
| Chilliwack | Fraser | 102,306 | 55,738 | 1,052 | 37 | 0.019 | 0.035 | 66.4 |
| Coquitlam | Fraser | 174,248 | 103,659 | 599 | 26 | 0.006 | 0.043 | 25.1 |
| Langley, City of | Fraser | 35,316 | 20,214 | 871 | 44 | 0.043 | 0.051 | 217.7 |
| New Westminster | Fraser | 92,433 | 58,645 | 565 | 43 | 0.01 | 0.062 | 73.3 |
| Surrey | Fraser | 700,459 | 412,964 | 3,335 | 230 | 0.008 | 0.069 | 55.7 |
| Kelowna | Interior | 165,200 | 95,475 | 2,032 | 89 | 0.021 | 0.044 | 93.2 |
| Penticton | Interior | 38,665 | 18,370 | 529 | 28 | 0.029 | 0.053 | 152.4 |
| Kamloops | Interior | 109,633 | 62,070 | 1,226 | 92 | 0.02 | 0.075 | 148.2 |
| Victoria | Island | 102,856 | 62,858 | 2,381 | 165 | 0.038 | 0.069 | 262.5 |
| Nanaimo | Island | 110,707 | 57,841 | 1,525 | 94 | 0.026 | 0.062 | 162.5 |
| Prince George | Northern | 84,905 | 49,322 | 1,758 | 109 | 0.036 | 0.062 | 221 |
| North Vancouver, City of | Vancouver Coastal | 67,308 | 41,589 | 400 | 25 | 0.01 | 0.062 | 60.1 |
| Richmond | Vancouver Coastal | 242,966 | 139,917 | 391 | 25 | 0.003 | 0.064 | 17.9 |
| Vancouver, City of | Vancouver Coastal | 756,008 | 493,285 | 9,564 | 527 | 0.019 | 0.055 | 106.8 |
There has been discussion that the COVID-19 pandemic elevated the overdose crisis by increasing incidence and, in turn, deaths. This section applies the DPIE framework to assess how incidence, population at risk, and intervention effectiveness contributed to changes before and after the onset of COVID-19. During the pre-COVID-19 period (2016–2019), death rates declined in Interior (−14.7%), and Island (−4.8%), whereas Northern Health experienced a large increase (+32.9%). Vancouver Coastal saw a modest increase (+6.0%), while Fraser Health experienced little change during this period.
Incidence increased in all regions, most sharply in Northern (+52.7%), with notable increases in Vancouver Coastal (+30.3%). Population at risk changed little, generally between +2% and +5.7%, indicating that worsening outcomes were driven primarily by overdose dynamics rather than demographic change. Intervention effectiveness improved in all health authorities; however, in Northern Health and Vancouver Coastal, improvements in intervention effectiveness were not strong enough to offset the increased incidence rate and the population at risk, leading to increased death counts. See Appendix 1, Table A1 for details.
The post-COVID period (2020–2023) reveals a more troubling shift. Death rose sharply in Northern Health (+218%), Interior (+122.6%), and Island (+110.4%). These increases were driven overwhelmingly by steep rises in incidence combined with worsening intervention effectiveness. Fraser experienced the smallest increase in deaths (+12.4), followed by Vancouver Coastal (+23.9%). See Appendix 1, Table A2.
Figure 2 presents heatmaps of percentage changes in overdose-related indicators by health authority for the pre-COVID period (2016–2019) and the post-COVID period (2020–2023). In the pre-COVID period, changes in deaths were modest and, in several regions, negative, despite moderate increases in the population at risk and incidence rates. Intervention effectiveness increased in all areas, more than offsetting increases in the population at risk and incidence rates, except for Northern Health and Vancouver Coastal. In contrast, the post-COVID period exhibits large increases in death rates across all health authorities, particularly in the Northern, Interior, and Island regions, accompanied by sharp increases in incidence and worsening intervention effectiveness, while growth in the population at risk remained comparatively small. The health authorities with the smallest increases in death rates were Fraser (12.4%) and Vancouver Coastal (+23.9%).
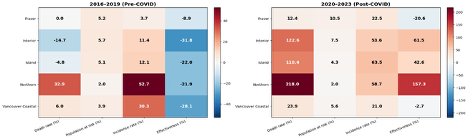
Figure 2: Percentage changes in overdose deaths, population at risk, incidence, and effectiveness by health authority before COVID-19 (2016–2019) and after COVID-19 (2020–2023). Values shown are percentage changes; components are related multiplicatively (Figure generated by the author using Spyder 6)
In summary, the Northern, Interior, and Island Health Authorities experienced the largest relative post-COVID increases in deaths, while Fraser and Vancouver Coastal exhibited smaller relative increases. Effectiveness improved post-COVID in Fraser, indicating improved survival conditional on overdose, but worsened in Northern, Interior, and Island. Overall, incidence increased in all health authorities except Vancouver Coastal, reinforcing that rising exposure to toxic drugs remains the dominant factor associated with increasing mortality.
Between 2023 and 2024, overdose death rates declined across all health authorities despite continued growth in the population at risk. Incidence rates fell in every region, while changes in effectiveness were mixed and comparatively modest. Consistent with the multiplicative DPIE framework, the decline in deaths reflects a reduction in incidence that offsets increases in the population at risk and changes in effectiveness. Table 3 provides a summary of percentage changes based on the DPIE framework components.
| Health Authority | Death (%) | Population at Risk (%) | Incidence rate (%) | Effectiveness (%) |
|---|---|---|---|---|
| Fraser | -8.4 | 5.0 | -0.3 | -13.0 |
| Interior | -8.2 | 4.4 | -18.3 | 5.7 |
| Island | -8.8 | 3.5 | -15.3 | 3.1 |
| Northern | -6.8 | 4.0 | -8.2 | -2.6 |
| Vancouver Coastal | -5.2 | 3.0 | -11.2 | 3.0 |
Note. Percentage changes are computed as \(r_{t,i} = ln \, ln \frac{R_{t,i}}{R_{t-j,i}} * 100\), where \(R_{t,i} = P_{t,i}, I_{t,i}, E_{t,i}\) for each health authority i between 2023 and 2024. Incidence rates are computed at the health-authority level as total overdose cases divided by total population at risk. Death rates are computed as total deaths divided by total population at risk. Because DPIE is multiplicative, percent changes in P, I, and E add to the percent change in D. The exact relationship is \(g_{D} = g_{P} + g_{I} + g_{E}\).
Preliminary (Jan–Aug 2025) counts suggest that the decline in drug deaths is continuing in most health authorities, especially Northern, with Interior, Island, and Vancouver Coastal also tracking below 2024 levels. Fraser is the exception, where the Jan–Aug 2025 pace is slightly above 2024. Because 2025 is incomplete at the time of this writing and seasonality matters, these comparisons should be treated as provisional.
Applying the DPIE Identity (Deaths = Population at Risk × Incidence × Effectiveness) across British Columbia’s five health authorities reveals important regional differences in overdose mortality trends. The findings show that areas with higher population risk and rising exposure to increasingly toxic drug supplies tend to experience higher death rates. Moreover, variations in the effectiveness of harm reduction measures, such as access to naloxone, supervised consumption sites, and healthcare integration, are reflected in the differing rates of decline or persistence of overdose deaths across the health authorities.
Programs offering a regulated safe supply and expanding supervised consumption sites have been effective in reducing acute overdose mortality. However, access remains uneven across municipalities, particularly in rural and Indigenous communities that are underserved. Furthermore, stigma, restrictive eligibility criteria, and regulatory barriers continue to limit the reach of these initiatives (Government of British Columbia, 2024).
The results also suggest that the health authorities in British Columbia’s Lower Mainland appear more effective at mitigating opioid-related mortality among the at-risk population. These patterns may reflect better integration of harm reduction services, more accessible urban infrastructure, and greater availability of complementary supports such as housing, primary care, and addiction treatment. However, it is important to recognize that these are aggregate-level findings, and there may be considerable variation in outcomes across municipalities within each health authority. In contrast, regions outside the Lower Mainland show higher mortality despite equal or greater site coverage, highlighting the influence of broader structural and contextual factors, such as geographic dispersion, stigma, and service fragmentation, on health system performance.
Additional drivers include socioeconomic stressors such as poverty, unemployment, trauma, and unstable housing, all of which increase vulnerability to substance use initiation (Dasgupta et al., 2018). The COVID-19 pandemic exacerbated these vulnerabilities by disrupting access to health and social services (Tobias et al., 2024). Social isolation and the increased toxicity of the drug supply during lockdown periods also contributed to record-high overdose deaths. Although efforts have been made to restore and expand post-pandemic services, the crisis revealed critical weaknesses in the resilience of harm reduction and healthcare systems when in-person services were temporarily non-existent or unavailable. The disruption of in-person services demonstrated how critical support resources are for individuals who rely on them, ultimately affecting how the health care system responds to overdose risks. The continued overprescription of opioids, along with insufficient public health outreach and education, also contributes to elevated rates of new cases. Collectively, these forces act as structural accelerants of the incidence rate, as shown in this research, reinforcing the need for coordinated prevention strategies alongside harm reduction and treatment to meaningfully reduce opioid-related mortality.
However, increases in the effectiveness of interventions could offset increases in the incidence rate and population at risk, but this depends on the accessibility and quality of harm reduction, treatment, and support services. Widespread access to naloxone, an opioid overdose reversal medication, significantly reduces fatality rates, particularly when deployed through community-based programs, first responders, and peer networks (Walley et al., 2013). Evidence-based medication-assisted treatment (MAT), such as buprenorphine and methadone, has also been shown to reduce mortality and improve long-term outcomes (Volkow et al., 2014). Furthermore, the expansion of safe consumption sites, complex care housing, Housing First models, and wraparound care services has been shown to improve treatment uptake, reduce overdose risk, and support retention in care, particularly among marginalized populations with complex needs (Pauly et al., 2021; Aubry et al., 2020; Latimer et al., 2017; Kennedy et al., 2019). Complex care housing has emerged as a promising strategy, particularly for individuals with overlapping challenges such as mental health disorders, substance use issues, and chronic homelessness. However, the scale of these initiatives remains insufficient relative to the size of the at-risk population, and long-term sustainability is uncertain without stronger funding commitments. These integrated supports help not only to offset the two other components of the DPIE framework, but also to counteract the social and systemic barriers, such as stigma, criminalization, and service fragmentation, that undermine treatment success. As such, improving effectiveness through accessible, coordinated care is just as vital as reducing incidence in mitigating overall opioid-related mortality.
Several critical gaps persist, including insufficient equitable access to safe supply and supervised consumption services; fragmented coordination across municipal, provincial, and federal levels of government; and insufficient integration of Indigenous-led strategies and culturally safe interventions. To achieve meaningful reductions in overdose mortality, policy must shift toward a systems-level, multisectoral, and long-term approach. Investment in upstream social determinants, expansion of harm reduction coverage, and partnerships with Indigenous communities are essential pillars of a sustainable response.
In the DPIE framework, the incidence rate is a critical component representing the number of new cases of opioid use per person within the population at risk. A rise in the incidence rate contributes directly to future mortality unless offset by improvements in the effectiveness of interventions. Several systemic and structural factors contribute to increased incidence. As one would expect, the availability and high potency of illicit synthetic opioids, particularly fentanyl, have significantly elevated the risk of addiction and overdose (Ciccarone, 2019). In addition, the increase in illicit fentanyl supply imported from international sources, including China and Mexico, often in highly concentrated forms that are easily trafficked and mixed with other drugs, has contributed to increased premature mortality (DEA, 2020). In response, the U.S. government under President Trump imposed tariffs on Canadian and Mexican imports in 2025, citing fentanyl trafficking as a national emergency due to its role in killing tens of thousands of Americans annually (Reuters, 2025; U.S. Congress, 2025; White House, 2025). However, the crisis is not unique to the United States; Canada has also experienced substantial losses, with 53,308 apparent opioid toxicity deaths reported between January 2016 and June 2025 (Public Health Agency of Canada, 2025).
Canada has recently initiated a national strategy focused on enforcement, harm reduction, treatment, and prevention, including appointing a national “fentanyl czar” to strengthen disruption of production and trafficking (Government of Canada, Health Canada, 2025; Associated Press, 2025). British Columbia reports multi-year investments in mental-health and substance-use supports (Government of British Columbia, 2024). Indicators from 2023 to 2024 and into 2025 suggest early signs of improvement with deaths falling alongside lower incidence rates and improved intervention effectiveness.
DPIE is a valuable decomposition method for the toxic drug poisoning crisis and other public health issues. However, several limitations should be acknowledged. First, DPIE is an identity-based decomposition rather than a causal model. The framework does not establish cause-and-effect relationships but instead decomposes observed mortality data into its component factors. As such, references to “drivers” or “contributions” should be interpreted as dominant terms in the decomposition, not causal effects. Second, the population at risk is defined as individuals aged 19–59, reflecting the age group that accounts for most toxic drug poisoning deaths in British Columbia. Sensitivity checks using broader adult populations yield similar qualitative patterns, suggesting that the main findings are not driven by this age restriction. Third, the Effectiveness (E) component, interrupted as the case fatality rate (deaths per overdose case) is used as a proxy measure for the overall effectiveness of intervention. While this measure is informative and policy-relevant, it has limitations. It is sensitive to case ascertainment, evolving drug toxicity, emergency response times, and reporting practices. In addition, improvements in E, particularly in the post-COVID period, may occur alongside rising overdose incidence, as increases in the denominator (overdose cases) can outpace deaths. Consequently, improvements in effectiveness do not necessarily imply reduced system-wide strain or fewer overdoses overall. Finally, the analysis integrates multiple administrative data sources, including coroner records, emergency health service responses, population projections, and site counts. These sources are subject to revision and may not align perfectly across time or geography. Despite these uncertainties, the principal spatial and temporal patterns appear robust, and the DPIE framework remains a valuable tool for identifying and comparing the components of overdose mortality relevant to public health policy.
The toxic drug poisoning crisis in British Columbia remains a public health emergency. Although trends from the past year are promising, continued investment in long-term initiatives should remain a priority. The DPIE framework allows for analytical examination of the factors contributing to the crisis and helps identify the specific components that intensity the issue. This framework can be adopted by health agencies and policymakers to better understand the root causes of overdose deaths. The DPIE framework decomposes overdose mortality into three key components: population at risk, incidence rate, and intervention effectiveness. This provides a valuable and adaptable tool for interpreting current trends and predicting future outcomes for practitioners and policymakers. The framework also allows organizations, sectors, and governments to set goals and targets using an evidence-based approach. For example, a policy target might aim to reduce deaths by 20% below 2025 levels by 2030. The DPIE framework allows communities to effectively align measurable targets with tangible, long-term policy commitments, strengthening accountability and evaluation of progress.
The data demonstrate that certain health authorities have had more effective intervention responses than others, which may explain why some regions are more successful in reducing mortality through investments of harm reduction initiatives and wrap-around services. Issues such as stigma, fragmented services, housing instability, and mental health challenges continue to act as barriers that exacerbate the crisis. A key policy focus should involve shifting from a reactive to a proactive approach. Emergency responses save lives, but long-term prevention, treatment, and recovery measures must also be prioritized.
The toxic drug poisoning crisis is a complex issue, and many strategies exist to help limit the number of cases and deaths. However, for this issue to improve, it must be addressed through a multilayered approach which simultaneously addresses substance use, trauma, poverty, mental health, and physical health. All levels of government must work together to coordinate funding, policy support, and resources for early prevention initiatives. Health regions across British Columbia should consider adopting practices like the expansion of harm reduction services and substance use prevention programs, and make these resources and knowledge available through the public education systems and integrated curricula to ensure that the crisis is addressed at an early stage. Another strategy that addresses the interconnected issues simultaneously is complex care housing, as these facilities support multiple health and social needs under one roof. Navigating the toxic drug crisis is complex, but combining a quantitative approach (DPIE) to identify the key factors associated with overdose deaths, together with qualitative insights like wraparound solutions (education, harm reduction initiatives, and complex care housing), allows for a more effective response. Identifying the right tools, resources, and strategies is the first step toward creating meaningful and sustained impact.
The DPIE framework highlights two primary policy levers for reducing opioid-related mortality: lowering the incidence of overdoses (I) and improving the effectiveness of intervention (E). Reducing incidence requires upstream strategies such as prevention, safer supply initiatives, housing stability, and mental health supports that address the structural drivers of substance use. Improving effectiveness depends on rapid emergency response, widespread naloxone availability, accessible supervised consumption services, and integrated care for individuals with complex needs. The results suggest that focusing on only one lever is insufficient; sustained reductions in deaths require coordinated policies that simultaneously limit exposure to toxic drugs and increase survival when overdoses occur.
Future research can extend the DPIE framework in several directions. One avenue is to complement the current identity-based decomposition with causal designs, such as event studies or interrupted time-series analyses around the introduction of supervised consumption sites, naloxone programs, or safer supply initiatives. A second extension is to formalize the DPIE identity within a STIRPAT-style stochastic modelling framework, allowing deaths to be modeled as a function of population at risk, overdose incidence, and intervention effectiveness while estimating elasticities and statistical uncertainty. This approach would move the analysis beyond deterministic attribution and permit hypothesis testing regarding the sensitivity of deaths to changes in incidence and effectiveness. Future work could also link the framework to micro-level or subgroup data to explore heterogeneity across age groups, sex, Indigenous communities, and rural versus urban settings, as well as incorporate indicators of drug supply toxicity. Finally, this framework may also be adapted to other public health conditions, allowing researchers and policymakers to compare the effectiveness of healthcare systems across different communities or regions.
The author gratefully acknowledges Dr. Peter Tsigaris for his guidance, feedback, and support throughout this project. The author also thanks her peers in the Capstone course for their helpful comments and discussions; Mr. Keegan Lawrence of the Canadian Institute for Substance Use Research at the University of Victoria for his valuable feedback; and participants at the 2025 TRU Undergraduate Research Conference, where this work was presented. Appreciation is also extended to Ms. Dani Collins for copyediting and thoughtful editorial revisions. The author further acknowledges the use of ChatGPT (OpenAI) to assist with the initial Python code used for figure generation and with editorial improvements. All analysis, interpretation, and any remaining errors are the responsibility of the author.
Akunna, O., Nneka, U., Nkesi, O., John, A., Cordelia, O., & Ada, A. (2024). Negative implications of drug and substance use on mental health. International Neuropsychiatric Disease Journal, 21(4), 18–25. https://doi.org/10.9734/indj/2024/v21i4439
Alamri, A., Bawazeer, A., Almotiri, T., Alharbi, S., Alshammari, D., Alnasser, B., & Alswayeh, H. (2022). Legislation and policy reform to combat drug addiction. International Journal of Health Sciences, 6(S10), 1736–1742. https://doi.org/10.53730/ijhs.v6ns10.15082
Alsabbagh, Mhd. W., Cooke, M., Elliott, S. J., Chang, F., Shah, N.-U.-H., & Ghobrial, M. (2022). Stepping up to the Canadian opioid crisis: A longitudinal analysis of the correlation between socioeconomic status and population rates of opioid-related mortality, hospitalization and emergency department visits (2000–2017). Health Promotion and Chronic Disease Prevention in Canada, 42(6), 229–237. https://doi.org/10.24095/hpcdp.42.6.01
Associated Press. (2025, February 11). Canada appoints former Mountie as fentanyl czar to combat production of the dangerous opioid. https://apnews.com/article/bf20a0ad1dbcf19623dbd6a0f54567bf
Aubry, T., Nelson, G., & Tsemberis, S. (2015). Housing first for people with severe mental illness who are homeless: A review of the research and findings from the At Home/Chez Soi demonstration project. The Canadian Journal of Psychiatry, 60(11), 467–474. https://doi.org/10.1177/070674371506001102
Bahji, A., Socias, M. E., Bach, P., & Milloy, M. J. (2023). Implications of cannabis legalization on substance-related benefits and harms for people who use opioids: A Canadian perspective. Cannabis and Cannabinoid Research, 8(5). https://doi.org/10.1089/can.2023.0031
Barry, C. L., McGinty, E. E., Pescosolido, B. A., & Goldman, H. H. (2014). Stigma, discrimination, treatment effectiveness, and policy: Public views about drug addiction and mental illness. Psychiatric Services, 65(10), 1269–1272. https://doi.org/10.1176/appi.ps.201400140
BC Centre for Disease Control. (2024). Overdose prevention and supervised consumption sites. https://www.bccdc.ca/health-info/disease-types/drug-overdose-response
British Columbia Coroners Service. (n.d.). Unregulated drug deaths─Township of injury [Interactive Power BI dashboard]. Government of British Columbia. Retrieved December 24, 2025, from https://app.powerbi.com/view?r=eyJrIjoiYjlkYTNmZjEtNzVjYi00NTMzLWE5NmEtMjU4NjEzYTMyNjVjIiwidCI6IjZmZGI1MjAwLTNkMGQtNGE4YS1iMDM2LWQzNjg1ZTM1OWFkYyJ9
BC Emergency Health Services. (2023a). BCEHS paramedics respond to 25% more overdose/poisoning calls in 2023. http://www.bcehs.ca/about/news-stories/stories/2023-annual-overdose-response-data
BC Emergency Health Services. (2023b). Overdose & drug poisoning data. http://www.bcehs.ca/about/accountability/data/overdose-drug-poisoning-data#Overdose--call--volumes
British Columbia Emergency Health Services. (n.d.). MPDS card 23 events: Overdose response in BC communities (top communities, 2016–2024) [Data table]. BC Emergency Health Services. Retrieved December 24, 2025, from the British Columbia Emergency Health Services reporting system. https://www.bcehs.ca/about-site/Documents/Card-23-Top-Communities-2024-publicdf
BC Stats. (2024). Sub-provincial population projections: 2024 edition. https://www2.gov.bc.ca/gov/content/data/statistics/people-population-community/population/population-projections
Campbell, C., Chiu, K., & Sud, A. (2024). Methadone prescribing regulation for opioid use disorder in Canada: Evidence for an east–west policy divide. Healthcare Policy | Politiques de Santé, 19(3), 49–61. https://doi.org/10.12927/hcpol.2023.27228
Carrière, G., Garner, R., & Sanmartin, C. (2021). Understanding the socioeconomic profile of people who experienced opioid overdoses in British Columbia, 2014 to 2016. Health Reports, 32(2), 27–38. https://doi.org/10.25318/82-003-x202100200003-eng
Ciccarone, D. (2019). The triple wave epidemic: Supply and demand drivers of the US opioid overdose crisis. International Journal of Drug Policy, 71, 183–188. https://doi.org/10.1016/j.drugpo.2019.01.010
Ciucă Anghel, D.-M., Nițescu, G. V., Tiron, A. T., Guțu, C. M., & Baconi, D. L. (2023). Understanding the mechanisms of action and effects of drugs of abuse. Molecules, 28(13), 4969–4969. https://doi.org/10.3390/molecules28134969
Dasgupta, N., Beletsky, L., & Ciccarone, D. (2018). Opioid crisis: No easy fix to its social and economic determinants. American Journal of Public Health, 108(2), 182–186. https://doi.org/10.2105/AJPH.2017.304187
Delic, M. (2022). Different dimensions of wellness in drug addiction treatment. European Psychiatry, 65(S1), S829–S829. https://doi.org/10.1192/j.eurpsy.2022.2146
Drug Enforcement Administration [DEA]. (2020). 2020 national drug threat assessment. U.S. Department of Justice. https://www.dea.gov/documents/2021/03/02/2020-national-drug-threat-assessment
Ehrlich, P. R., & Holdren, J. P. (1971). Impact of population growth. Science, 171(3977), 1212–1217. https://doi.org/10.1126/science.171.3977.1212
Government of British Columbia. (2018). Population Estimates - Province of British Columbia. https://www2.gov.bc.ca/gov/content/data/statistics/people-population-community/population/population-estimates
Government of British Columbia. (2024). Escalated drug-poisoning response actions (factsheet). BC Gov News. https://news.gov.bc.ca/factsheets/escalated-drug-poisoning-response-actions-1
Government of Canada. (2024, September 13). Opioid- and stimulant-related harms in Canada. Health Infobase. https://health-infobase.canada.ca/substance-related-harms/opioids-stimulants/
Government of British Columbia. (2025). Complex care housing - Province of British Columbia. https://www2.gov.bc.ca/gov/content/health/managing-your-health/mental-health-substance-use/complex-care-housing
Government of British Columbia. (2025). Population estimates - Province of British Columbia. Gov.bc.ca. https://www2.gov.bc.ca/gov/content/data/statistics/people-population-community/population/population-estimates
Government of Canada, Health Canada. (2025, December 11). Federal actions on the overdose crisis. https://www.canada.ca/en/health-canada/services/opioids/federal-actions/overview.html
Hatt, L. (2022, January 6). The opioid crisis in Canada. https://lop.parl.ca/sites/PublicWebsite/default/en_CA/ResearchPublications/202123E
Hawke, L. D., Zhu, N., Relihan, J., Darnay, K., & Henderson, J. (2022). Addressing Canada’s opioid crisis: A qualitative study of the perspectives of youth receiving substance use services. Canadian Journal of Addiction, 13(2S), S39. https://doi.org/10.1097/CXA.0000000000000148
Hunnicutt, T. (2025, December 15). Trump signs executive order classifying fentanyl as ‘weapon of mass destruction’. Reuters. https://www.reuters.com/world/us/trump-says-he-will-sign-executive-order-classifying-fentanyl-weapon-mass-2025-12-15/
Irvine, M. A., Kuo, M., Buxton, J. A., Balshaw, R., Otterstatter, M., Macdougall, L., Milloy, M‐J., Bharmal, A., Henry, B., Tyndall, M., Coombs, D., & Gilbert, M. (2019). Modelling the combined impact of interventions in averting deaths during a synthetic‐opioid overdose epidemic. Addiction, 114(9), 1602–1613. https://doi.org/10.1111/add.14664
Kennedy, M. C., Hayashi, K., Milloy, M. J., Wood, E., & Kerr, T. (2019). Supervised injection facility use and all-cause mortality among people who inject drugs in Vancouver, Canada: A cohort study. PLoS Medicine, 16(11), e1002964. https://doi.org/10.1371/journal.pmed.1002964
MacDougall, L., Smolina, K., Otterstatter, M., Ko, M., Godfrey, D., Zhao, B., & Cheng, J. (2018). Development and characteristics of the provincial overdose cohort in British Columbia, Canada. International Journal for Population Data Science, 3(4). https://doi.org/10.23889/ijpds.v3i4.1033
McNeil, R., Fleming, T., Mayer, S., Barker, A., Mansoor, M., Betsos, A., Austin, T., Parusel, S., Ivsins, A., & Boyd, J. (2022). Implementation of safe supply alternatives during intersecting COVID-19 and overdose health emergencies in British Columbia, Canada, 2021. American Journal of Public Health, 112(S2), S151–S158. https://doi.org/10.2105/ajph.2021.306692
Ning, A., & Csiernik, R. (2022). Why has the opioid crisis remained unchanged in Canada? The limits of bio-scientific based policy approaches. Journal of Social Work Practice in the Addictions, 1–11. https://doi.org/10.1080/1533256x.2022.2071822
O'Donnell, J. K., Halpin, J., Mattson, C. L., Goldberger, B. A., & Gladden, R. M. (2017). Deaths involving fentanyl, fentanyl analogs, and U-47700—10 states, July–December 2016. Morbidity and Mortality Weekly Report, 66(43), 1197–1202. https://doi.org/10.15585/mmwr.mm6643e1
Panagiotoglou, D. (2022). Evaluating the population-level effects of overdose prevention sites and supervised consumption sites in British Columbia, Canada: Controlled interrupted time series. PLOS ONE, 17(3), e0265665. https://doi.org/10.1371/journal.pone.0265665
Public Health Agency of Canada. (2025, December 11). Opioid- and stimulant-related harms in Canada: Key findings. Health Infobase. Government of Canada. https://health-infobase.canada.ca/substance-related-harms/opioids-stimulants/
Runyon, S., & Shane, C. (2024). A missed opportunity: How the British Columbia Court of Appeal could have helped reform sentencing in the opioid crisis. Alberta Law Review, 61(3), 721–. https://doi.org/10.29173/alr2780
Smolina, K., Crabtree, A., Chong, M., Zhao, B., Park, M., Mill, C., & Schütz, C. G. (2019). Patterns and history of prescription drug use among opioid-related drug overdose cases in British Columbia, Canada, 2015–2016. Drug and Alcohol Dependence, 194, 151–158. https://doi.org/10.1016/j.drugalcdep.2018.09.019
Snowdon, J., & Choi, N. (2022). Unanticipated changes in drug overdose death rates in Canada during the opioid crisis. International Journal of Mental Health and Addiction, 22. https://doi.org/10.1007/s11469-022-00932-9
Tobias, S., Buxton, J. A., & Ti, L. (2024). Local impact from international crises: Unregulated drug toxicity during the COVID-19 pandemic in British Columbia, Canada. American Journal of Public Health, 114(6), 587–589. https://doi.org/10.2105/ajph.2024.307673
U.S. Congress, Congressional Research Service. (2025). Executive Order 14193 (IN12533). https://www.congress.gov/crs_external_products/IN/HTML/IN12533.html
VanSteelandt, A., Chang, G. Y. S., McKenzie, K., & Kouyoumdjian, F. (2024). Accidental substance-related acute toxicity deaths among youth in Canada: A descriptive analysis of a national chart review study of coroner and medical examiner data. Health Promotion and Chronic Disease Prevention in Canada, 44(3), 77–88. https://doi.org/10.24095/hpcdp.44.3.02
Volkow, N. D., Frieden, T. R., Hyde, P. S., & Cha, S. S. (2014). Medication-assisted therapies—Tackling the opioid-overdose epidemic. New England Journal of Medicine, 370(22), 2063–2066. https://doi.org/10.1056/NEJMp1402780
Vyas, R., Bailey, K., Vyas, N., & Compton, P. (2021). College students’ knowledge about opioids and implications for the opioid crisis. Journal of American College Health, 71(1), 1–7. https://doi.org/10.1080/07448481.2021.1881102
Waggoner, P. E., & Ausubel, J. H. (2002). A framework for sustainability science: A renovated IPAT identity. Proceedings of the National Academy of Sciences, 99(12), 7860–7865. https://doi.org/10.1073/pnas.122235999
Wakeland, W., Nielsen, A., Schmidt, T. D., & McCarty, D. (2022). Modeling the evolution of the US opioid crisis for national policy development. Proceedings of the National Academy of Sciences, 119(1), e2115714119. https://doi.org/10.1073/pnas.2115714119
Walley, A. Y., Xuan, Z., Hackman, H. H., Quinn, E., Doe-Simkins, M., Sorensen-Alawad, A., et al., & Ozonoff, A. (2013). Opioid overdose rates and implementation of overdose education and nasal naloxone distribution in Massachusetts: Interrupted time series analysis. BMJ, 346, f174. https://doi.org/10.1136/bmj.f174
White House. (2025, February). Fact sheet: President Donald J. Trump imposes tariffs on imports from Canada, Mexico, and China. https://www.whitehouse.gov/fact-sheets/2025/02/fact-sheet-president-donald-j-trump-imposes-tariffs-on-imports-from-canada-mexico-and-china/
Wong, J., Westenberg, J., Mathew, N., Azar, P., & Krausz, R. M. (2021). Risk and protective factors for opioid overdose during the COVID-19 pandemic. European Psychiatry, 64(S1), S825–S825. https://doi.org/10.1192/j.eurpsy.2021.2179
Yao, X., Rama, A.-A., Mazzitelli, J., McFaull, S. R., & Thompson, W. (2024). A mixed methods study on poisoning and injury-related emergency department visits associated with opioids in Canada, 2011 to 2022: Data from the Canadian hospitals injury reporting and prevention program. BMC Public Health, 24(1). https://doi.org/10.1186/s12889-024-20016-8
| Health Authority | Death rate (%) | Population at Risk (%) | Incidence rate (%) | Effectiveness (%) |
|---|---|---|---|---|
| Fraser | 0.0 | 5.2 | 3.7 | -8.9 |
| Interior | -14.7 | 5.7 | 11.4 | -31.8 |
| Island | -4.8 | 5.1 | 12.1 | -22.0 |
| Northern | 32.9 | 2.0 | 52.7 | -21.9 |
| Vancouver Coastal | 6.0 | 3.9 | 30.3 | -28.1 |
Note. Percentage changes are computed as \(r_{t,i} = ln \, ln \frac{R_{t,i}}{R_{t-j,i}} * 100\), where \(R_{t,i} = P_{t,i}, I_{t,i}, E_{t,i}\) for each health authority between 2016 and 2019. Incidence rates are computed at the health-authority level as total overdose cases divided by total population at risk. Death rates are computed as total deaths divided by total population at risk. Because DPIE is multiplicative, percent changes in P, I, and E add to the percent change in D. The exact relationship is \(g_{D} = g_{P} + g_{I} + g_{E}\).
| Health Authority | Deaths (%) | Population at Risk (%) | Incidence rate (%) | Effectiveness (%) |
|---|---|---|---|---|
| Fraser | 12.4 | 10.5 | 22.5 | -20.6 |
| Interior | 122.6 | 7.5 | 53.6 | 61.5 |
| Island | 110.4 | 4.3 | 63.5 | 42.6 |
| Northern | 218.0 | 2.0 | 58.7 | 157.3 |
| Vancouver Coastal | 23.9 | 5.6 | 21.0 | -2.7 |
Note. Percentage changes are computed as \(r_{t,i} = ln \, ln \frac{R_{t,i}}{R_{t-j,i}} * 100\), where \(R_{t,i} = P_{t,i}, I_{t,i}, E_{t,i}\) for each health authority between 2020 and 2023. Incidence rates are computed at the health-authority level as total overdose cases divided by total population at risk. Death rates are computed as total deaths divided by total population at risk. Because DPIE is multiplicative, percent changes in P, I, and E add to the percent change in D. The exact relationship is \(g_{D} = g_{P} + g_{I} + g_{E}\).

This work is licensed under a Creative Commons
Attribution-NonCommercial-ShareAlike 4.0
International license